Table of ContentsClose
The research lab of Sam Stephens, PhD, studies the pancreatic islet beta-cell, which regulates whole-body metabolism through the release of insulin. Failure of the beta-cell to maintain insulin production is a major contributor to the transition from insulin resistance to Type 2 diabetes. Stephens, an assistant professor of internal medicine, is interested in understanding how the beta-cell regulates the production of insulin and how this process becomes dysregulated during the development of diabetes. In a recent paper in the journal Function using models of Type 2 diabetes, the team identified a specific defect in the packaging of insulin into storage vesicles that can be overcome using a novel antioxidant treatment. This work is currently funded by the Department of Defense and was recently awarded a pilot and feasibility grant from the University of Iowa Fraternal Order of Eagles Diabetes Recent Center.
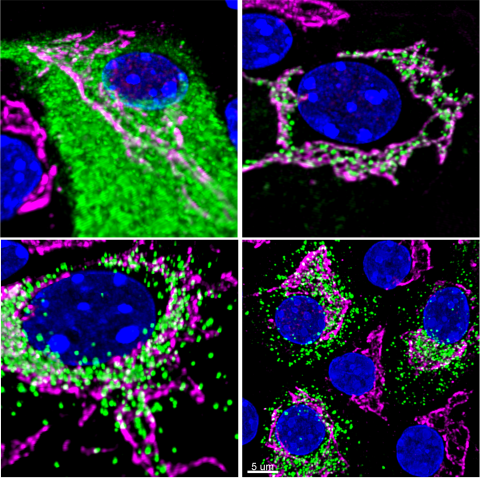
The Stephens lab has developed a reporter system to visualize insulin production in live pancreatic islet beta-cells. Insulin (green) is synthesized and folded within a large cellular compartment called the endoplasmic reticulum (top left), which occupies a large part of the beta-cell’s volume. Within about 30 minutes, insulin is transported to another organelle, the Golgi (magenta), for sorting and packaging (top right). About 30 min after entering the Golgi, insulin packages, called secretory vesicles, leave the Golgi (bottom left). Insulin vesicles are then maintained in the storage pool (bottom right) until they are released into the bloodstream in response to a rise in blood sugar.
Images submitted by graduate student Cierra Boyer, who works in the Stephens lab.
