With the conventional first-line drug for early-stage bladder cancer in severe shortage, new therapies developed at Iowa are poised to lead a new wave of care.

As a young investigator on the Harvard Medical School faculty in the 1990s, Michael O’Donnell, MD, began to question the conventional approach to treating early-stage bladder cancer.
The regimen for high-risk cases had remained the same since the 1970s: tumor resection followed by intravesical bacillus Calmette-Guerin (BCG), an immunotherapy derived from cow tuberculosis. Why BCG worked was not well understood, but it succeeded in about 60% of patients. For the rest, the only option left was radical cystectomy—removal of the bladder.
Bladder cancer is one of the most common cancers in the U.S. About 75% of patients are diagnosed with early-stage disease, known as superficial or non-muscle-invasive bladder cancer (NMIBC), which is usually highly treatable. The cancer cells are in the inner lining of the bladder but have not yet spread to the muscle layers.
Yet, as the millennium approached, O’Donnell saw that the chance of recurrence, progression, bladder removal, and death caused by this treatable disease hadn’t changed in more than 20 years. Investigations at that time typically focused on single-agent approaches that repeatedly proved less effective and more toxic than BCG.
The field of study appeared to be stuck in a rut. O’Donnell was ready to try something different. In 2000, during a trip to the University of Iowa to deliver a lecture, O’Donnell received an intriguing offer from Richard Williams, MD, then chair of the UI Department of Urology: Come to Iowa and build a world-class bladder cancer program.
O’Donnell seized the opportunity to put his ideas into practice. He left Boston for Iowa City.
“The whole point is to cure as many cancers without removing bladders,” says O’Donnell, now the Richard D. Williams Professor of Urology and director of urologic oncology for UI Health Care. “It struck me as odd that in the rest of oncology, cancers were being treated with multi-agent chemotherapy, yet in urology we persisted in using single drugs and hoping that they would somehow miraculously give large effects. And it wasn’t happening.”
Bladder Cancer Facts
Bladder cancer is the sixth most common cancer in the U.S. overall. In men, it’s the fourth most common cancer.
Estimates for 2023:
- New bladder cancer diagnoses: 82,290 (62,420 in men, 19,870 in women)
- Bladder cancer deaths: 16,170 (12,160 in men, 4,550 in women)
Top risk factors:
- Smoking (causes about half of all cases)
- Workplace exposure to chemicals
- Gender (much more common in men)
- Age (much more common in people over 55)
Source: American Cancer Society
Success of multi-agent approach makes Iowa a destination for care
O’Donnell began studying chemotherapy combinations that could maximize efficacy while minimizing toxicity. Sticking to that approach over two decades, he has devised an astonishing six new intravesical chemotherapy treatments, giving urologists an unprecedented number of new options to save bladders and keep patients cancer-free.
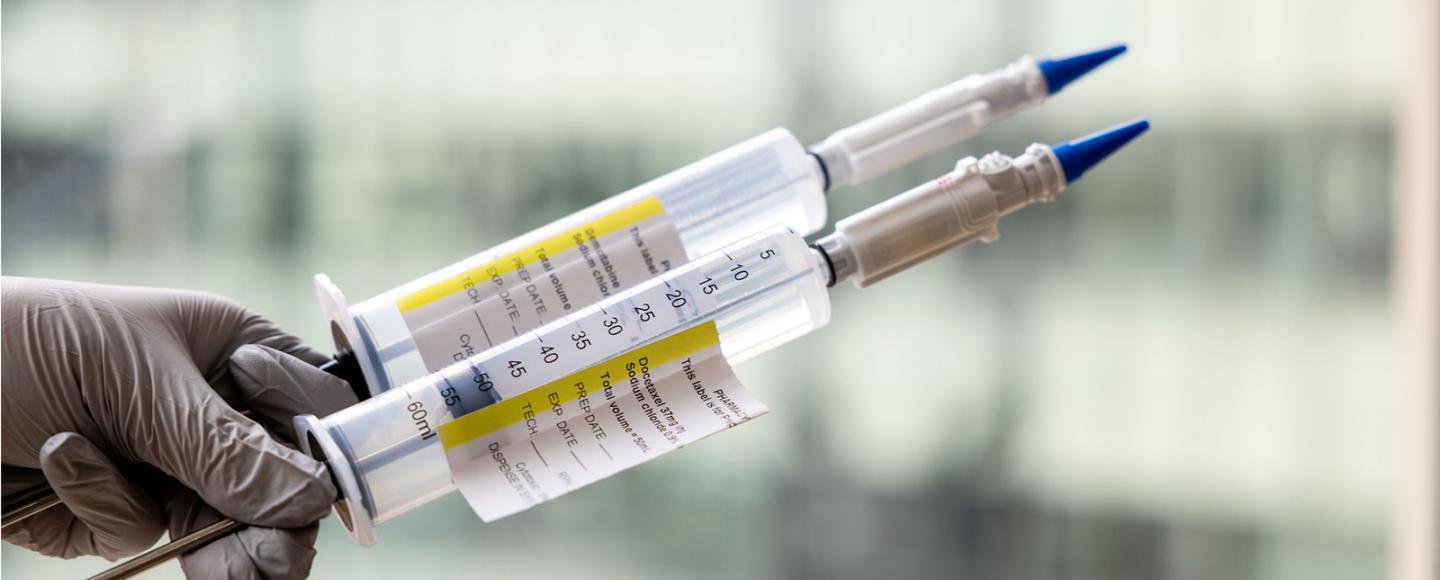
The centerpiece of that body of work is a regimen of sequential doses of two low-cost generics: gemcitabine and docetaxel (gem/doce) (pictured above). In 2015, O’Donnell and his UI colleagues published the first study of the therapy’s effectiveness. They described their success using gem/doce to treat 45 patients who had failed multiple courses of BCG. Two years after treatment, 34% of those patients—patients who otherwise would have been advised to have their bladders removed—were cancer-free.

Urologists at leading cancer centers across the country, including Johns Hopkins, Harvard, and MD Anderson, were now turning to Iowa to learn about using gem/doce after BCG failures. At the same time, bladder cancer patients from around the world were traveling to UI Holden Comprehensive Cancer Center after learning about O’Donnell’s groundbreaking work.
As the UI program refined and improved the gem/doce regimen, O’Donnell began recommending the new therapy to most of his patients as a first-line therapy in place of BCG, which was often in short supply because of manufacturing problems. When BCG supplies went into a critical, long-term, worldwide shortage in 2019, the UI bladder cancer program weathered the disruption because it had already moved beyond sole reliance on BCG.
O’Donnell believes all programs should strive to do the same, and the UI program is paving the way for them.
“We have the most advanced early-stage bladder cancer program in the world,” he says.
A potential new direction, eagerly anticipated

Vignesh Packiam, MD, cultivated a deep interest in bladder cancer during residency training at the University of Chicago and fellowship training in urologic oncology at Mayo Clinic. Like O’Donnell did a generation before him, Packiam arrived at the UI in 2020 eager to lead meaningful change.
“Mike O’Donnell hit a home run, finding, for the first time, something that works as well, and possibly even better, than BCG,” says Packiam, clinical assistant professor of urology. “It offers a radical change in how we do things. For someone young and motivated to make advances in research and help patients, this was the place to be.”
Upon arrival, Packiam was tasked with highlighting the results of treating patients with gem/doce. He was senior author of a milestone study published in 2022 in the Journal of Urology that analyzed follow-up data from 107 patients with high-risk NMIBC who received gem/doce as first-line therapy, bypassing BCG altogether. It was the largest study ever conducted of such a population, and it reported that 82% of those patients remained cancer-free at two years, significantly higher than BCG’s two-year, cancer-free rate, historically about 60 to 65%.
The findings highlighted the promise of gem/doce as an effective replacement for BCG for high-risk disease. With BCG still nearly unobtainable for the foreseeable future, more and more urologic oncologists are looking to use gem/doce.
Last year, Packiam co-authored an article in AUA News reporting on a survey of North American urologic oncologists on gem/doce usage. Of 198 respondents, 71% had prescribed gem/doce in the previous year for patients who had failed BCG. The authors estimated that at least 1,300 NMIBC patients now receive the UI-pioneered regimen each year.
“Everyone knows what gem/doce is now,” Packiam says. “And almost everyone is using it or wants to use it.”
BRIDGE Trial: Gem/doce vs. BCG
To date, all the studies reporting on gem/doce outcomes have been retrospective, analyzing past patient data, and most of that data has come from UI Hospitals & Clinics patients. A UI study directly comparing gem/doce to BCG, published in in JAMA Network Open in February 2023, was also a retrospective analysis of UI patient data, and it showed that gem/doce was better than BCG in preventing recurrence of high-risk cancer in a population of 312 patients. In early 2023, however, a group of cancer research centers launched the BRIDGE clinical trial, a highly anticipated nationwide study that will recruit 870 NMIBC patients and conduct the first prospective, controlled, randomized comparison of BCG and gem/doce.
“There’s already a huge waiting list of centers eager to get started,” says Packiam, who along with O’Donnell helped develop the study’s protocol. “There’s a lot of excitement about this trial.”
Packiam serves as the UI’s principal investigator for the study, and he’s also one of the trial’s designated advocates, recruiting new centers and helping them get the protocol up and running.
“If this trial shows the results that we think it will, that gem/doce is as effective as BCG, it has the potential to completely change how we’ve treated NMIBC since before 1980,” Packiam says.

The latest: Alternative bladder cancer treatment emerges amid worldwide shortage of standard care BCG
A new study from the University of Iowa finds that gem/doce is better tolerated than BCG and is better at preventing high-grade cancer recurrence in patients with non-muscle invasive bladder cancer (NMIBC).
The first steps toward personalized bladder cancer care
The BRIDGE trial likely won’t be completed for seven or eight years. Packiam is ready now to start moving bladder cancer care into its next era, building on the success of the UI program’s preceding 20 years of discovery. He already sees two promising directions that he is passionate about following.
The first is continuing the UI’s early work to personalize NMIBC care through genomics. With multiple treatments available, patients will receive better care if their doctors know in advance which therapy will likely work best for them.
“We’re looking at new biomarkers—in the urine, in the blood, or in the tumor—to predict if a patient is going to respond better to a particular treatment,” Packiam says. “I don’t think any other center is as well-equipped as we are to do that. We have the most experience and a huge bio bank of specimens.”
His second passion is the development of a treatment-agnostic framework that clinicians can use to design care plans that optimize quantity and quality of life.
“We can do all these new things to save a bladder,” Packiam says. “But will the bladder be functional? What will the patient’s quality of life look like, even after the cancer is gone? I think we’re in the best position to look at that new question, and I’m very interested in leading the charge.”
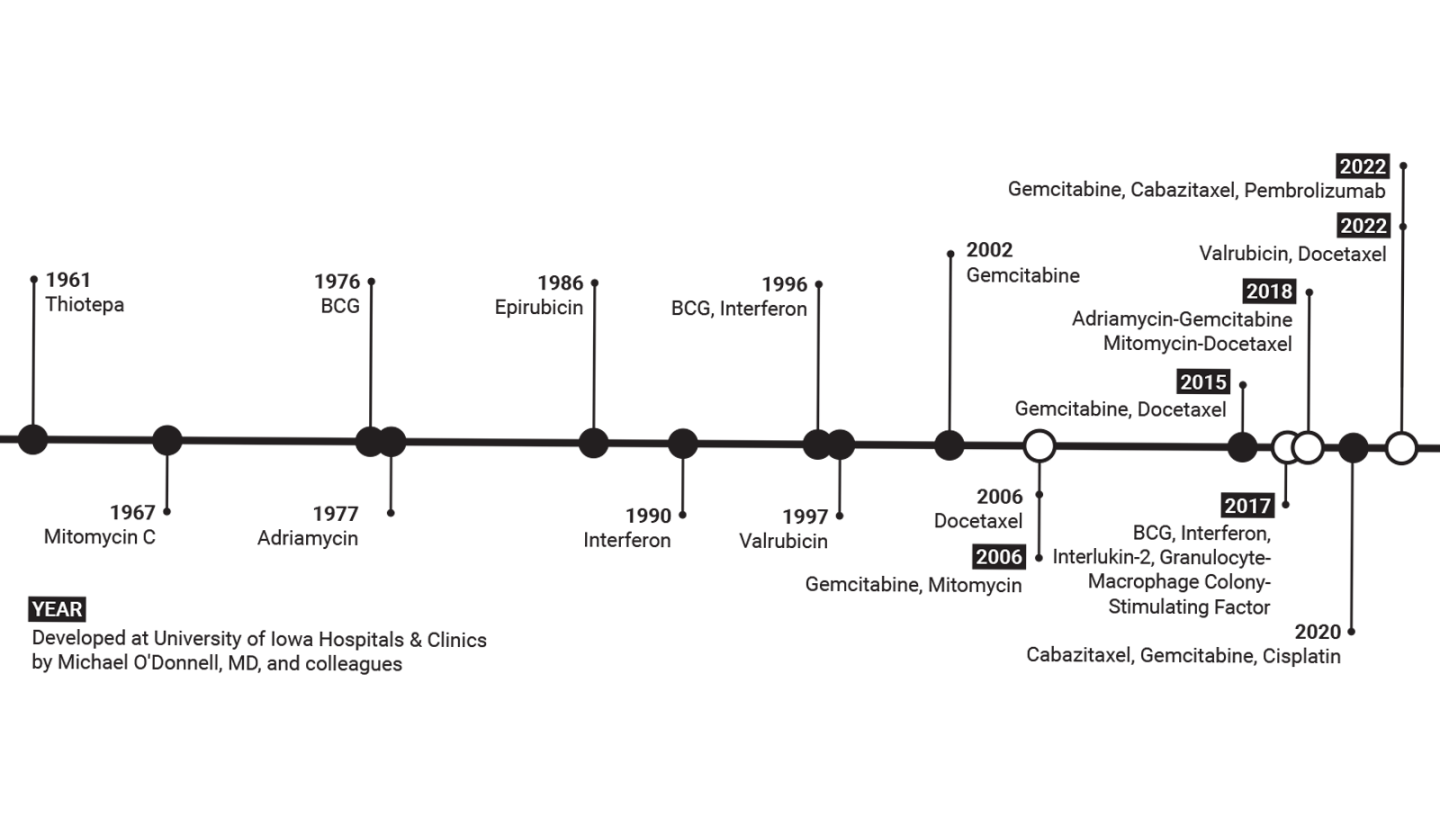
Timeline of intravesical treatments for NMIBC (by publication year)
| Year | Name of Treatment |
|
1961 |
Thiotepa |
| 1967 | Mitomycin C |
| 1976 | BCG |
| 1977 | Adriamycin |
| 1986 | Epirubicin |
| 1990 | Interferon |
| 1996 | BCG + Interferon |
| 1997 | Valrubicin |
| 2002 | Gemcitabine |
| 2006 | Docetaxel |
| 2006* | Gemcitabine / Mitomycin |
| 2015* | Gemcitabine / Docetaxel |
| 2017* | Quad Immuno BCG (BCG, Interferon, Interlukin-2, Granulocyte-Macrophage Colony-Stimulating Factor) |
| 2018* | Quad Chemo (Adriamycin-Gemcitabine Mitomycin-Docetaxel) |
| 2020 | Gemcitabine / Cabazitaxel /Cisplat |
| 2022* | Gemcitabine /Cabazitaxel/Pembro |
| 2022* | Valrubicin / Docetaxel |
*= developed at University of Iowa Hospitals & Clinics by Michael O’Donnell, MD, and colleagues
A program—and a career—defined by reimagining what’s possible
As O’Donnell surveys the bladder cancer program that Williams challenged him to build, he sees it on a trajectory even he couldn’t have imagined back in 2000.
“This is what you want your career to turn into,” he says. “You want it to take on a life of its own.”
To illustrate the driving force that led to that, O’Donnell recalls a conversation that could have been lifted straight from the script of a TV medical melodrama.
In 2013, he had run out of options for a patient who had a small tumor in his bladder. The best available treatments—including gem/doce—had failed to kill the cancer cells. The only realistic choice left was radical cystectomy.
The patient refused.
“He wanted a better choice,” O’Donnell says. “He looked me in the eye and said, ‘I have a tumor the size of a postage stamp, and you’re telling me I have to lose my bladder? No. Come up with something else.’”
To most ears, that might have sounded like an unreasonable demand. For O’Donnell, it was a rallying cry.
“A lot of the work I do is the direct result of heroic patients who stood up for what they believed in and put their trust in me to try something new,” he says.
O’Donnell responded by devising another novel intravesical chemotherapy combination—valrubicin and docetaxel—that, to his knowledge, had never been used to treat NMIBC.
It worked. The patient kept his bladder and a year later was cancer-free. O’Donnell has since used that regimen to treat dozens of patients who otherwise would have had no choice but to opt for a cystectomy.
With that kind of inspiration, along with the generosity of the John and Carol Walter Family Foundation and other donors who support his program’s research, O’Donnell considers it his duty to keep pushing against the boundaries of what is possible.
“If you believe in the motto of this institution—Changing Medicine, Changing Lives—you have to put your money where your mouth is,” O’Donnell says. “Otherwise you’re just doing the same thing as everybody else. Who wants to be average?”
Photos by Liz Martin.

UNIQUE CARE AT IOWA
Our experts provide comprehensive evaluation and treatment in the clinic setting as well as surgical interventions for all urologic system diseases and disorders.

GEM/DOCE RESEARCH LEAVES LASTING IMPRINT ON YOUNG PHYSICIAN’S CAREER
Ryan Steinberg, MD (18R), remembers when, early in his urology residency training at UI Hospitals & Clinics, he grasped just how unusual a program he had joined.
“When you’re green and you’re still learning, you assume that the way the patients are cared for at your training site is the way that everyone does it,” says Steinberg, now clinical assistant professor of urology at the UI. “Then, further along, I was learning and reading, and I started searching the literature, and I thought, ‘Why can’t I find anything about the treatment we give here?’”
Steinberg’s mentor was Michael O’Donnell, MD. The treatment was gem/doce for NMIBC following BCG failure. It wouldn’t make its first appearance in the literature until 2015—with Steinberg listed as first author. Other papers would follow, including one that is still cited in FDA guidelines for industry development of bladder cancer drugs.
That’s heady stuff for a trainee.
“I’m a fourth-year resident, and I’m the first author on a paper cited by the FDA to help guide clinical trial design,” Steinberg says. “That was pretty special.”
He would go on to complete two years of fellowship training in endourology and minimally invasive surgery at the University of Texas-Southwestern, returning to the UI in 2020 as a faculty member with a focus on kidney stones and minimally invasive surgery.
“Ryan is misguided because he went into stones,” O’Donnell says with a laugh. “But he was the guy who got things done. He was such an important part of getting our work out there for the first time.”
The experience left an indelible imprint on Steinberg’s career.
“Doing that research and understanding the impact of that work was a major point of growth in my career,” he says. “Dr. O’Donnell’s guidance, and the autonomy he allowed me, definitely helped lead me down the path to academic medicine, and I still have so much pride in that work I did as a resident. It’s very gratifying to continue to be so closely associated with it.”

MAKING THE MOST OF THE UI’S SUMMER RESEARCH FELLOWSHIP
Long before his first day as a student in the Carver College of Medicine, Ian McElree had a research mentor and was working on a highly influential study.
McElree was participating in the college’s Summer Research Fellowship Program, which provides a stipend of up to $6,000 for pre-M1s and M1s interested in learning scientific investigation from the ground up.
His mentor, Vignesh Packiam, MD, says McElree went well beyond the research requirements of the summer program—he brought an inquisitive and rigorous mindset to maximize the impact of the work. McElree’s project culminated in the landmark 2022 publication in the Journal of Urology that described the largest study of patients with high-risk NMIBC who received gem/doce as first-line therapy.
“Ian took the initiative in doing an excellent job with retrospective chart review, identifying patients, medications, outcomes, side effects, and working with me and Dr. O’Donnell throughout the process,” Packiam says. “It’s a huge credit to him, and it’s a huge credit to the opportunity that the Summer Research Fellowship offers.”
When he returned for a second summer, McElree worked on the follow-up project that led to the milestone February 2023 publication in JAMA Network Open that described the head-to-head comparison of BCG and gem/doce.
“Very few urologic studies make it into that journal,” Packiam says. “Most trainees would shy away from shooting for a high-impact journal like that. Ian didn’t blink at that challenge, which paid off.”
McElree has presented at major national conferences, including the annual meetings of the American Urological Association and the Society of Urologic Oncology.
“I’ve been so fortunate to have this chance to explore a career as a physician-scientist,” McElree says. “I’m discovering new ideas, sharing exciting findings, and taking part in changing the future of medicine.”
McElree (right) is pictured with Packiam at the Society of Urologic Oncology’s annual conference.