Table of ContentsClose
Growing up in a small Iowa town, Andrea Austin (11MD) shadowed her local physician assistant, who mentored and encouraged her to eventually go into medicine herself.
The events of Sept. 11, 2001, reinforced her interest in becoming a medical professional and led her to pursue a career as a military physician and practice emergency medicine.
“It was very formative for me,” says Austin, who was a high school sophomore on 9/11. “I thought, ‘Those emergency physicians are really out in an area that’s very challenging.’”
Austin later entered medical school at the University of Iowa Carver College of Medicine with a scholarship from the U.S. Navy. She completed residency training at the Naval Medical Center in San Diego.
Fifteen years after 9/11 and nine years after being commissioned as a Naval Officer, Austin deployed to Iraq and Kuwait as an emergency physician for seven months. While in Iraq, she primarily cared for Iraqis injured by improvised explosive devices and gunfire.
The hospital she worked in had only X-ray and ultrasound imaging capabilities and a very limited lab, Austin says.
“I really feel like I got to use my whole training,” she says. “I saw the most severely injured patients I’ve ever seen. We took excellent care of people, had very high survivability, even with what we would consider—coming from an American hospital—very limited capability. You can actually take really great care of trauma patients even under those conditions.”
The events of 9/11 prompted the military to partner with the emergency medicine residency program at the Los Angeles County (LAC) + USC Medical Center to begin training medical professionals in dealing with trauma. When she returned from her deployment, Austin became the first female emergency medicine physician to be stationed at the Navy Trauma Training Center at LA County + USC.
“It was such an honor to be trusted with teaching military people before they go into challenging circumstances and really being their guide to getting ready to take care of severely injured trauma patients,” Austin says.
Currently an emergency medicine physician working at Sharp Grossmont Hospital in San Diego and simulation educator at the Naval Postgraduate School, Austin will assume a new role this spring as the simulation director for emergency medicine at Temecula Valley Hospital in Temecula, California.
Simulation is a primary academic interest of Austin’s and involves using both manikins and actors to teach medical students and residents procedural and clinical reasoning skills before they’re at a patient’s bedside. She also helps students learn how to maintain and build upon those skills as medicine changes.
“The protocols we use—around CPR and other procedures—change, and so simulation is a really great way to practice those skills in a safe environment in which we’re 100% sure there will be no patient harm,” Austin says. “What I really like about it is it's really centered on patient safety and empowering clinicians to reach their peak performance and have excellence in all aspects of their career.”
Her new position is also part of a new simulation program that she’s spearheading, Austin says.
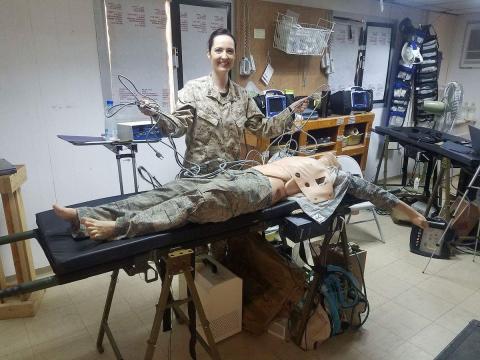
“I’m excited to take this secret sauce of my last 10 years and stir it all together to hopefully make the most engaging and rewarding simulation experience for this new group of residents,” she says.
Austin says veterans’ health is a passion of hers, and she aims to help not only military but also non-military people understand that veterans will show up in emergency departments with depression, anxiety, post-traumatic stress disorder, and a variety of other afflictions stemming from their military service for many years to come.
She added that suicide among veterans is a huge issue, with approximately 20 veterans committing suicide each day.
“I only deployed once, but I took care of Marines that deployed six or seven times, and I can guarantee you that nobody that deploys six or seven times comes back unharmed, physically or mentally,” she says. “Part of being a good citizen is bearing witness to the suffering that they had and supporting them to live the best life that they can, knowing that they volunteered, and they went.”
Austin has also partnered with Linda Lawrence, MD, to create the company Revitalize, offering individual and group coaching for female physicians looking to rejuvenate their career.
“That’s really a culmination of the last decade,” she says. “I’ve gone through some periods of burnout; I’ve worked at places that haven’t always been a great fit. But medicine needs us to stay in this profession, and there’s a lot of demands on physicians, so learning how to be better in tune with what you need to show up fully for your patients—it's hard.”
She’s grateful to be from and have attended medical school at Iowa, Austin says, because she believes the primary care foundation of medicine was a great bedrock to build upon. Citing her own experience studying abroad in India as a medical student, Austin says interacting with different cultures and health care systems makes a physician more flexible.
“I’ve worked in rural hospitals, I’ve worked in Iraq, I’ve worked in the biggest, fanciest institutions that have every subspeciality you can think of, and that’s made me extremely adaptable,” Austin says. “My first inclination when I hear about doing something different isn’t that it’s wrong. It’s, ‘Let me learn more about that. Maybe there’s something I can learn from this.’”

We'd love to hear from you
Send us updates and news at medicine-alumni@uiowa.edu
