Table of ContentsClose

The latest news from UI Health Care
News Roundup
University of Iowa Health Care clinicians have received a grant for a multifaceted quality improvement project using artificial intelligence (AI) to identify more individuals with advanced prostate cancer who would benefit from genetic testing.
As many as 10% to 15% of patients with advanced prostate cancer have germline mutations, yet genetic testing rates for men with advanced prostate cancer hover around 15% nationally.
“If there is a genetic mutation that is shared among siblings or children, we can do more targeted screening and intervene earlier,” says urologic oncologist Kenneth Nepple, MD, the project’s principal investigator.
The Iowa team will configure an AI tool called Evidently to automatically alert physicians if a patient may be eligible for genetic testing. From there, they will use a variety of outreach tools to let patients know they are eligible, why genetic testing is important, and how to get tested.
“We’re already using the tool to identify patients during clinical encounters, and will only improve our capabilities from here,” Nepple says. The project is backed by a collaborative funding initiative launched by the American Urological Association, Pfizer, and Astellas.

The Carver College of Medicine’s brain bank, known as the Iowa Neuropathology Resource Laboratory, is now part of the National Institutes of Health’s NeuroBioBank (NBB) network.
Since 2013, the NBB has centralized resources aimed at collecting and distributing postmortem human brain tissue to understand conditions of the nervous system. The NBB network distributes samples to researchers studying neurological, developmental, and psychiatric disorders.
As the seventh brain bank in the NBB network, the Iowa Neuropathology Resource Lab (INRL) will bank 100 brains per year, with 50 more dedicated to grant-supported projects. Their responsibilities include performing MRIs and three-dimensional scans, histology workups, and associated data collection to make well-characterized, postmortem human tissue available for free through the NBB to investigators across the country. In turn, the INRL will receive $1.4 million in funding for the first year of the contract.
The INRL currently consists of over 500 donated brains, most of which come from a partnership with the Iowa Office of the State Medical Examiner and the Iowa Donor Network. The repository at Iowa will be the only such brain bank in the Midwest, comprising a unique representation of specimens from a rural population and giving researchers a look into generational environmental exposures that are otherwise difficult to obtain.
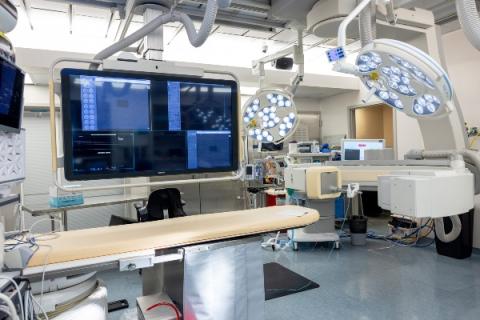
Patients scheduling cardiac electrophysiology procedures now have the option to receive care at University of Iowa Health Care’s downtown campus in Iowa City.
The reopening this past October of the EP lab — part of the cardiac catheterization lab at the downtown campus— is part of a commitment to enhancing community health care while expanding access and reducing wait times for important procedures. The downtown campus has continuously offered cardiology and interventional cardiology services, but EP services had been suspended before the downtown campus became part of UI Health Care in early 2024.
The EP lab at the downtown campus has been upgraded and outfitted with new technology and equipment. Procedures available at the downtown location include implanting pacemakers and implantable cardioverter defibrillators as well as cardiac ablations and cardioversions.
The electrophysiology team will continue to see all patients for clinic appointments at the UI Health Care’s university campus. With the reopening of this lab, patients will be scheduled at either campus for EP procedures, depending on the first available opening.
University of Iowa Health Care leaders have announced appointments to several key positions over the past several months:

Kyle Anson, JD, MBA, became associate vice president for human resources in November 2025, a position he had held on an interim basis since June 2024. Anson has held several leadership roles in human resources at UI Health Care. During his interim tenure, he guided the integration of Mission Cancer + Blood, oversaw the onboarding and alignment of staff at the North Liberty campus, and helped launch a new leadership development program.

Melissa Whisler, MBA, MHA, was appointed executive director of UI Health Care’s Transformation Office on a permanent basis in November 2025 after serving in this role since July. She will lead and support alignment between strategy, implementation, and operational efforts across the enterprise. Whisler joined UI Health Care in 2008 and has served in clinical department and administrative leadership roles. Most recently, she was UI Health Care’s administrative chief of staff for the clinical enterprise.

J. Joshua Wilda, MPA, joined UI Health Care in September 2025 as vice president for information systems and chief information digital officer. He leads UI Health Care’s Health Care Information Systems team and oversees information technology services, including technical support, applications development, and clinical applications across the entire health care system. Wilda previously served as chief digital and information officer at University of Michigan Health–Regional Network.
Expanded unit meets growing need for specialized neonatal care
University of Iowa Health Care Stead Family Children’s Hospital welcomed patients and families to its newly expanded neonatal intensive care unit (NICU) in early March. A built-out space on Level 7 of the children’s hospital allows the nationally ranked neonatology program to care for more premature and high-risk infants and meet Iowa’s growing need for highly specialized newborn care.
Stead Family Children’s Hospital has some of the highest survival rates in the country for extremely premature infants. It is home to Iowa's only nationally ranked Level 4 NICU — the highest level recognized by the American Academy of Pediatrics — which means it is equipped to care for the tiniest and most critically ill babies with the greatest range of neonatal services.
“Expanding our NICU represents a major milestone for families across Iowa and for our children’s hospital,” says Denise Jamieson, MD, MPH, UI vice president for medical affairs and the Tyrone D. Artz Dean of the Carver College of Medicine. “As access to maternal and newborn care remains limited in many communities, we are seeing more complex pregnancies and babies who need our advanced neonatal services. These new spaces ensure we can expand access while continuing to deliver the highest level of care for our most vulnerable patients.”

Designed for high-acuity neonatal care, training
The opening of Level 7 marks the halfway point for a two-part expansion within Stead Family Children’s Hospital that includes Level 8, which is slated for completion later this year. Built in 2017, the Stead Family Children’s Hospital’s seventh and eighth floors were originally constructed as shell spaces for future expansion. The completion of Level 7 will host 32 NICU beds, plus dedicated support spaces, family waiting areas, and provider work rooms that will increase capacity while enhancing the care environment for patients, families, and team members.
“We have a team of world-class neonatologists, and this expansion allows us to continue providing world-class care,” says Patrick McNamara, MB, BCh, division director of neonatology. “The completion of Level 7 gives our teams the space and infrastructure they need to respond quickly, work efficiently, and deliver highly specialized care to the most premature and medically complex newborns in Iowa and the region.”
The Level 7 NICU is designed to support the complex, team-based care required for critically ill and extremely premature newborns. In addition to increasing bed capacity, the new environment improves workflows, proximity of specialty services, and communication among multidisciplinary teams.
"Our goal is not only to help babies survive, but to give them every opportunity to thrive —strengthening collaboration and advancing the specialized care that defines our program,” says Brady Thomas, MD, NICU medical director.
Centralized support services improve efficiency
Among the NICU’s specialized services is neonatal hemodynamics, which monitors a baby’s cardiovascular health to deliver safer and more accurate care. UI Health Care neonatal specialists are at the forefront of implementing this advanced imaging technique while also educating and training NICU teams from around the world.
“To successfully care for such tiny, fragile babies, we need the most advanced technology, and these new spaces are designed to support the infrastructure needs of such essential equipment,” says Danielle Rios, MD, MS, director of the neonatal hemodynamics program.

An existing drug currently used to treat glaucoma, altitude sickness, and seizures may also have potential for preventing relapse in opioid use disorder, according to a study by University of Iowa Health Care researchers.
The researchers, led by John Wemmie (96MD-PhD, 00R), focused on the drug acetazolamide (AZD) because it blocks the activity of a brain enzyme called carbonic anhydrase 4 (CA4). Wemmie’s team had previously discovered that inhibiting CA4 in mice significantly reduced the brain changes that occurred after cocaine withdrawal. Blocking the CA4 enzyme also reduced drug-seeking behavior and relapse in the mice.
In their new study, published in Neuropsychopharmacology, the researchers found that disrupting CA4 genetically or with a single dose of AZD also prevented adverse changes in the brain and behavior after withdrawal from oxycodone, a commonly abused opioid. They showed that blocking CA4 reduced the strengthening of drug-related synaptic connections and also reduced the desire to seek the drug.
“AZD is already approved for human use and has a good safety profile, which raises the exciting possibility that it might be readily repurposed to reduce drug-seeking and relapse in opioid use disorder and other substance use disorders,” says Wemmie, a professor of psychiatry in the Carver College of Medicine
The Carver College of Medicine announced the latest cohort of the Stead Family Scholars Program in fall 2025.
Funded by a generous donation from Iowa natives Jerre and Mary Joy Stead, the program supports promising early-career investigators whose bold research ideas have the potential to transform science and medicine. The scholars receive $125,000 per year for three years to pursue new, unexplored ideas that promise consequential discoveries. They also benefit from specialized professional development programs in leadership and communication.
The program has already begun to pay dividends, allowing scholars in previous cohorts to expand their programs, pivot into new methods, and publish their findings.
The 2025 Stead Family Scholars:
James Byrne, MD, PhD, Assistant Professor
Department of Radiation Oncology

Byrne’s lab focuses on translational engineering to solve complex biomedical problems through innovative, high-risk research approaches. Funding from the Stead Family Scholars program will support his team's investigation of novel radioprotective strategies aimed at reducing treatment-related toxicities and improving quality of life for cancer patients undergoing radiation therapy.
Stephanie Gantz, PhD, Assistant Professor
Department of Molecular Physiology and Biophysics

Gantz’s research pursues a fundamental understanding of how and when the ubiquitous and enigmatic delta-1 glutamate receptors signal in the brain, with the goal of uncovering therapeutic potential of targeting these receptors to treat human diseases. With this funding, Gantz plans to examine the relationship between brain pH and delta-1 glutamate receptor function as it pertains to cognitive function and neuropsychiatric symptoms.
Jeremiah Johnson, PhD, Associate Professor
Department of Microbiology and Immunology

Johnson (11PhD) studies how the bacterial pathogen Campylobacter jejuni infects the gastrointestinal tract, induces inflammation, and causes tissue damage. While infection from the pathogen typically resolves without incident, recent studies have provided evidence that a variety of autoimmune and inflammatory disorders can occur following Campylobacter infection. Support through the Stead Family Scholars program will allow his team to examine whether inflammation during pediatric infection is different and whether this has unique effects on the pediatric gastrointestinal tract.
Hua “Linda” Sun, MD, PhD, Associate Professor
Stead Family Department of Pediatrics–Nephrology, Dialysis, and Transplantation

Sun (17R) studies a heavy-duty transport system inside kidney cells, powered by the motor protein cytoplasmic dynein. Her team was the first to discover that in diabetes, this transport network goes off course — misdelivering critical cargo, damaging cells, and ultimately causing the loss of the kidney’s filtering units. With the support of this fund, Sun’s lab is uncovering how this breakdown rewires cellular metabolism and scrambles gene activity. The group is also performing drug screening to identify compounds that can restore dynein-mediated trafficking, offering potential new treatments. Sun's ultimate goal is to develop innovative therapies that can restore — or even protect — kidney health from the earliest stages of diabetic stress, especially in children and adolescents.
In the News
Selected quotes from Carver College of Medicine faculty featured online and in the news media.
“While I don’t think these measures play a large role in addressing different forms of alopecia, I will often recommend specific regimens if I see that they are deficient.”
In a U.S. News & World Report article on “Best Vitamins for Hair Growth,” alopecia expert Ali Jabbari, MD, PhD, professor and chair of the Department of Dermatology, notes that he has specific recommendations when it comes to supplementing vitamins and micronutrients when these are found to be deficient.

“I hear all the time how someone’s having stroke symptoms, and their reaction is, ‘Well, I’m going to take a nap and see if they go away.’”
Enrique Leira, MD, MS, professor in the Department of Neurology and head of UI Health Care’s Comprehensive Stroke Center, tells Time magazine that people often don’t recognize stroke symptoms and delay seeking care. Difficulty with speech — slurring words, speaking slowly, or having trouble finding the right words — is one symptom patients should never ignore and seek care immediately, Leira says.

“Humidifiers can provide modest relief, but they’re not a cure-all.”
In a New York Times story about the use of humidifiers in the winter, Likhita S., MBBS, a sleep medicine specialist and clinical assistant professor in the Department of Neurology, notes that humidifiers can relieve skin tightness or itchiness, but serious skin issues like eczema will likely require other treatments. She adds that while a humidifier may keep you from waking up with a dry nose or throat, it won’t treat an underlying sleep disorder.

Paper Trail
Notable manuscripts recently published by Carver College of Medicine faculty.
Nature
Rete ridges form via evolutionarily distinct mechanisms in mammalian skin
Thompson SM, Yaple VS, Searle GH, Phan QM, Makkar J, Cheng X, Liu R, Pulawska-Czub A, Yanke C, Williams NM, Busch IV, Duong TT, Corneto MV, Jordan ZS, Roy D, Salmon AB, Slayden OD, Hermann BP, Stoltz DA, Welsh MJ; UW Birth Defects Research Laboratory; Glass IA, Kobielak K, Nie Q, Jin S, Jansen HT, Ciccarelli M, Plikus MV, Driskell IM, Driskell RR. Nature 2026 Feb 4. doi: 10.1038/s41586-025-10055-5. Epub ahead of print.
JAMA
Trends in Vitamin K Administration Among Infants
Scott K, Miller E, Culhane JF, Greenspan J, Handley SC, Lo JY, Knake LA, McKenney KM, Burris HH, Dysart K. JAMA 2026 Jan 20;335(3):272-274. doi: 10.1001/jama.2025.21460.
The Lancet
Risk markers for sudden unexpected death in epilepsy: an observational, prospective, multicentre cohort study
Ochoa-Urrea M, Luo X, Vilella L, Lacuey N, Omidi SJ, Hupp NJ, Talavera B, Hampson JP, Rani MRS, Tao S, Li X, Miyake CY, Cui L, Hampson JS, Chaitanya G, Vakilna YS, Sainju RK, Friedman D, Nei M, Allen L, Scott CA, Oliveira J, Gehlbach B, Schuele SU, Ogren JA, Harper RM, Diehl B, Bateman LM, Richerson GB, Yamal JM, Zhang GQ, Devinsky O, Lhatoo SD. Lancet 2025 Oct 4;406(10511):1497-1507. doi: 10.1016/S0140-6736(25)01636-8. Epub 2025 Sep 17. Erratum in: Lancet 2025 Oct 4;406(10511):1472. doi: 10.1016/S0140-6736(25)01970-1.
